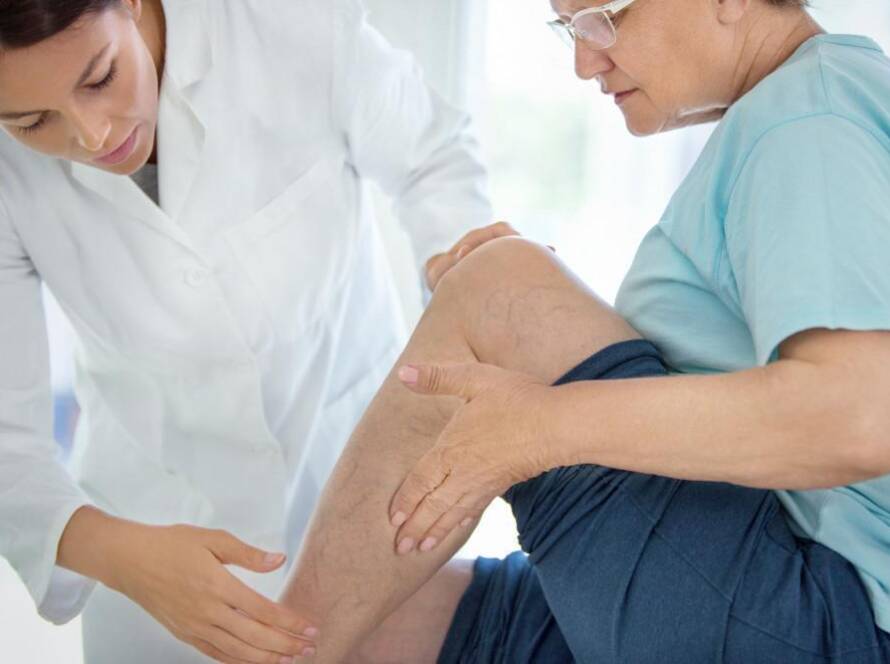
About 15% of people with diabetes develop a nonhealing skin wound (ulcer) on their legs or feet according to estimates cited by the American Podiatric Medical Association. And about 6% of them eventually require hospitalization due to infection or other complications.
Vascular specialist, Dr. Nirav Patel and our team at Premier Vascular In Yonkers and Jackson Heights, New York, provide exceptional care for nonhealing wounds. He is Chief of Vascular Surgery and Medical Director of the Wound Healing Center at St. John’s Riverside Hospital.
Our top-level wound care expert shares the following about diabetic ulcers.
What is a diabetic ulcer?
Most commonly appearing on the lower legs or bottoms of the feet, diabetic ulcers are open sores or wounds that simply do not heal. The ulcerations may become quite painful and make it hard to stand or walk.
An ulcer may start as a:
- Blister
- Cut
- Crack in the skin
- Callus
- Area of redness
- White spot
Without proper treatment, a diabetic ulcer may lead to a life-threatening infection that can spread to the bone (osteomyelitis) or into the bloodstream (sepsis). This can eventually result in amputation.
What causes diabetic ulcers?
Issues associated with long-term or uncontrolled diabetes are often at the root of diabetic foot and leg ulcers.
Diabetic peripheral neuropathy (nerve damage), for instance, is a common complication of diabetes that affects your ability to accurately sense pain.
Typically beginning in the lower legs and feet, peripheral neuropathy can make it impossible to feel a blister, skin abrasion, or cut on the foot. Without attention, the area can quickly become infected or develop into an ulcer.
Peripheral arterial disease (PAD) is another issue that often develops in those with diabetes. PAD causes narrowing of the arteries that supply blood to your legs, limiting the availability of oxygen and other critical nutrients your body uses to heal skin wounds and fight infection.
Varicose veins and other conditions that affect your veins, the blood vessels that transport blood back to the heart, also increase your risk of developing leg swelling and skin changes that may lead to ulcers.
Skin made more fragile by diabetes is also susceptible to friction wounds caused by walking in tightly fitting shoes or those without adequate cushioning. Self-treatment of corns and calluses can also cause wounds that develop into foot ulcers.
How do you treat diabetic foot and leg ulcers?
Our team at Premier Vascular offers a full range of wound care services that, depending on the nature of your ulcer, may include:
- Compression therapy to reduce swelling
- Wound cleaning and debridement
- Advanced dressings
- Oral or topical antibiotic therapy
- Bioengineered tissue substitutes
- Negative pressure wound therapy
- Off-loading to eliminate pressure
Dr. Patel can also provide treatment to help address the underlying cause of your ulcer, such as minimally invasive angioplasty for PAD. He also develops a home care strategy that speeds wound healing and helps prevent future issues.
Don’t wait to schedule a visit with Dr. Patel at Premier Vascular if you’re struggling with diabetic-related skin, nerve, or vascular changes. Call one of our New York offices or click the “request appointment” button.